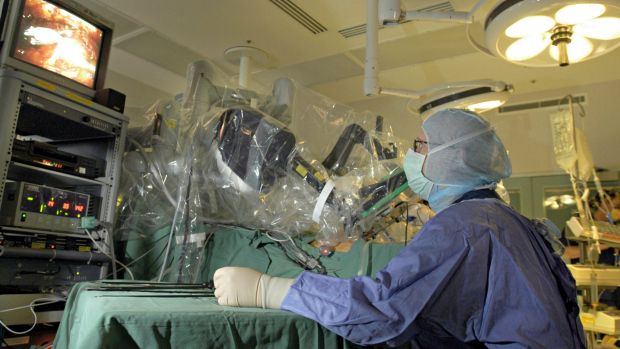
Expensive robotic prostate surgery, marketed as “ground breaking”, “revolutionary” and “nerve sparing”, has been found to be no better at preserving men’s urinary continence and sexual function than traditional surgery.
A landmark Australian study made the finding after comparing the advanced surgery, which can cost more than $10,000, with traditional open surgery three months post operation.

The first trial to directly compare the two procedures for prostate removal randomly split 308 men into two groups. All the operations were led by two experienced surgeons at the Royal Brisbane and Women’s Hospital who had done at least 200 prostate operations.
When the two groups were assessed at three months, there was no difference in urinary or sexual function, or in post-operative complications such as infections. Patients who had the open surgery lost more blood during the procedure but none of them needed transfusions.
“Many clinicians claim the benefits of robotic technology lead to improved quality of life and oncological outcomes [but] our randomised trial, the first of its kind, found no statistical difference in quality of life outcomes between the two groups at 12 weeks follow-up,” said lead author of the study Professor Robert ‘Frank’ Gardiner from the University of Queensland. Patients who had open surgery had a longer hospital stay post surgery and experienced more pain doing day to day activities one week after the operation but, on average, both groups spent the same number of days off work.
He said patients are now being followed up for two years to fully assess the longer-term outcomes, including cancer survival.
“In the meantime, patients should choose an experienced surgeon they trust and with whom they have a rapport, rather than basing their decision on a specific surgical approach,” Professor Gardiner said.
President of the Urological Society of Australia and New Zealand Mark Frydenberg said the study, published in The Lancet medical journal on Wednesday, showed both techniques were “equally effective”.
Professor Frydenberg said “patients without access to robotic surgery should not feel in any way disadvantaged or be concerned they will have an inferior outcome”.
“Our view is that both robotic and open surgery are very valid treatments for prostate cancer but what is of most relevance to outcomes is the skill and experience of the surgeon,” he said.
Worldwide, one million men are diagnosed with prostate cancer each year, including about 18,000 Australian men, and surgery is often recommended as treatment. While two out of three men are likely to never be diagnosed with cancer again, the surgery can cause incontinence and erectile dysfunction.
Since the first robot-assisted prostate removal (prostatectomy) was reported in 2000, the procedure has been widely adopted in western countries, including Australia where some surgeons charge thousands of dollars in out of pocket fees. Many hospitals have paid about $3 million for the robots which cost about $300,000 to service each year.
The robot uses a high magnification 3D camera that allows a surgeon to see inside a patient’s abdomen through a keyhole incision. The robot has four arms which hold the camera and other surgical instruments. These arms are controlled by the surgeon who sits in the same room, but away from the patient.
For the older “open” procedure, an incision is usually made through the lower abdomen to remove the prostate gland, although sometimes the incision is made between the rectum and the base of the penis.
Professor Ara Darzi, of Imperial College London, said many doctors were waiting “with anticipation” for the next results of the study when the men will be assessed one year after their surgery.
“It will be the interpretation of the longer-term functional and oncological outcomes that reveals the full implications of this study for clinical practice,” he wrote in The Lancet.