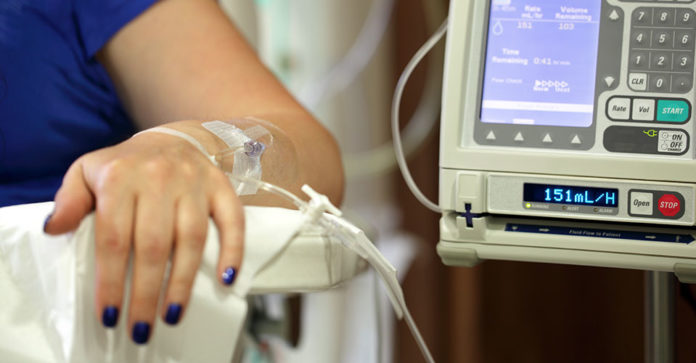
Chemotherapy has saved countless lives and is a mainstay of cancer care. But for some patients, it can also do more harm than good, according to a new study published in the Journal of the American Medical Association (JAMA) Oncology, which found that giving chemotherapy to people with end-stage cancer was associated with poorer quality of life and no medical benefit.
The findings challenge widespread clinical practice as well as accepted treatment guidelines, and underscore the need for clinicians to re-evaluate the common use of chemotherapy at the end of patients’ lives, the authors say.
“Oncologists may presume there to be no harm in giving dying patients chemotherapy, but these data point to more harm than benefit,” said study author Dr. Holly Prigerson, from Weill Cornell Medical College in New York City.
The study followed a group of more than 300 patients with advanced cancer who had an average of four months to live. About half of the patients were receiving what’s known as palliative chemotherapy when the study began. Palliative chemotherapy is generally given to people who have fewer than six months to live, according to the researchers. The hope is that the treatment, which involves delivering potent chemicals into the body to kill cancer cells and shrink tumors, will ease symptoms and extend survival.
But this new study found it had neither of these effects.
‘If the purpose was to improve the quality of life, these findings really raise questions about the legitimacy of that claim’
Among the patients who at the start of the study were generally healthiest and most active, palliative chemotherapy use was associated with worse quality of life in their last week of life and showed no benefit to overall survival. Those who were less healthy at the study’s outset experienced no net effect from the treatment, in quality of life or survival.
“These data show that incurable cancer patients with a limited life expectancy who use chemotherapy are likely to impair the quality of their remaining days,” Dr. Prigerson said. “Not only did chemotherapy not benefit patients regardless of performance status, it appeared most harmful to those patients with good performance status.”
In other words, the chemotherapy made the patients feel worse without providing any significant benefit for their cancer. “If the purpose was to improve the quality of life, these findings really raise questions about the legitimacy of that claim,” Dr. Prigerson told CBS News.
The authors suggest that “guidelines regarding chemotherapy use in patients with terminal cancer may need to be revised to recognize the potential harm of chemotherapy use in patients with progressive metastatic disease.”
Groups like the American Society of Clinical Oncologists (ASCO) recently advised doctors to be more judicious with their use of chemotherapy in terminal patients. ASCO’s guidelines recommend limiting it to relatively healthy patients who can withstand the toxic treatment and potentially overcome side effects. But this new study “demonstrates that palliative chemotherapy does not appear to palliate symptoms even in the most robust patients who can tolerate chemotherapy,” Dr. Prigerson said. “It raises questions about the rationale for such aggressive, burdensome care.”
It’s important to point out that these results only apply to end-stage terminal cancer patients, not to all patients with advanced or metastatic cancer. And the findings definitely do not imply that chemotherapy is ineffective when it comes to improving survival rates for patients with advanced tumors. Just the opposite is true, actually: chemotherapy typically confers the most benefits to patients with complicated or advanced cancers.
For example, advances in chemotherapy over the past couple of decades have increased survival in patients with liver metastases from 6 months to close to two years. Chemotherapy has also been shown to significantly improve survival rates for a range of other complex cancers such as metastatic colorectal cancer, non-small cell lung cancer, pancreatic cancer, advanced head and neck cancer, hereditary breast cancer, and metastatic prostate cancer. And for hematologic malignancies like leukemia, chemotherapy is attributed with increasing 10-year survival rates from less than 10% to over 80% since the 1970’s.
‘Equating treatment with hope is inappropriate’
Ultimately, the decision about how long to continue care, including chemotherapy, is up to each cancer patient, but Dr. Prigerson hopes that her research helps to better inform those choices in coming years. Recent studies have shown, for example, that despite explanations from their doctors, many cancer patients still believe that more rounds of chemo will provide some benefit to them, and are therefore—and understandably—reluctant to stop receiving therapy. But at some point, the evidence shows, more treatment is not better.
That may be especially true of patients with end-stage cancer who are still relatively healthy and not feeling sick. For them, additional chemotherapy will likely make them weaker, not to mention eat up more of the precious time they have left traveling to and from infusion centers. Dr. Prigerson plans to continue the study to better understand the dynamics of how decisions about treatments are made toward the end of life, but in the meantime hopes the latest findings at least convince doctors to reconsider how they advise their terminal patients about end-stage chemotherapy.
In an accompanying editorial, two physicians from the Oregon Health and Science University argued that there are only two reasons to give a patient chemotherapy, which can be time-consuming, expensive, and have side effects: it should either extend their lives or make their lives better. The new study, they write, brings “troubling” data to one of the most difficult problems in cancer treatment. It also challenges one of the biggest prevailing ideas about cancer: the analogy to a battle.
The study suggests “that equating treatment with hope is inappropriate,” Drs. Charles Blanke and Erik Fromme wrote. “Even when oncologists communicate clearly about prognosis and are honest about the limitations of treatment, many patients feel immense pressure to continue treatment. Patients with end-stage cancer are encouraged by friends and family to keep fighting, but the battle analogy itself can portray the dying patient as a loser and should be discouraged.”