Researchers conducted a prospective randomized controlled clinical trial at Bern University Hospital in Switzerland to compare a laparoscopic procedure with a mini-laparotomy for insertion of a peritoneal catheter during ventriculoperitoneal (VP) shunt surgery. The deciding factor was the rate of shunt malfunction. Although overall shunt failure rates did not differ substantially between patients in the two surgery groups, the authors identified a significant reduction in the rate of distal (abdominal) shunt failure in patients in whom laparoscopy was used. Detailed findings of the clinical trial are reported and discussed in “Laparoscopically assisted ventriculoperitoneal shunt placement: a prospective randomized controlled trial” by Philippe Schucht, MD, Vanessa Banz, MD, PhD, and colleagues, published today online, ahead of print, in the Journal of Neurosurgery.
Background: Hydrocephalus is a condition in which there is excessive accumulation of cerebrospinal fluid (CSF) in chambers of the brain known as ventricles. If left uncorrected, the excess CSF can exert pressure on critical brain structures, causing the patient to experience cognitive, visual, or motor deficits; seizures; or even death. Ventriculoperitoneal (VP) shunts are frequently placed to redirect excess CSF away from the brain and into the peritoneal cavity in the abdomen, where the body can absorb it. Most VP shunts consist of a catheter that is placed in one of the ventricles in the brain, a one-way valve that draws excess CSF away from the ventricles, and a second catheter placed under the skin that carries this excess fluid down to the peritoneal cavity.
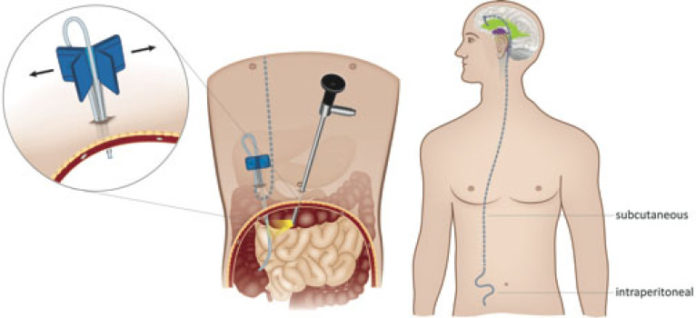
Placement of a VP shunt is a two-part operation. In addition to surgery to the head, where the ventricular catheter and pump are placed, an incision must be made in the abdomen for placement of the end of the peritoneal catheter. The focus of this study is on two abdominal procedures: mini-laparotomy, which involves open surgery, and a laparoscopic approach, a less invasive procedure in which a small puncture hole is made through which the end of the peritoneal shunt catheter is inserted into the peritoneal cavity and positioned with the aid of a tiny laparoscopic camera.
Present Study: The authors state that 120 adult patients were randomized to undergo a laparoscopic procedure or mini-laparotomy for insertion of a peritoneal catheter during initial or revised VP shunt surgery for hydrocephalus. Data were collected around the time of surgery and 6 and 12 months later. The primary end point of this study was the overall rate of shunt malfunction (failure or complication related to any part of the shunt system) at 12 months postoperatively. Secondary end points included the overall rate of shunt malfunction at 6 weeks and 6 months postoperatively, the rate of distal shunt malfunction (failure or complication related to the peritoneal catheter) at all three time points, the lengths of the operation and hospital stay, and the rate of morbidity.
Findings of previous retrospective studies had indicated the superiority of laparoscopic shunt placement over mini-laparotomy in the rate of distal shunt malfunction (and consequently the overall rate of shunt malfunction) as well as the durations of surgery and hospitalization. The authors conducted this prospective clinical trial to collect stronger evidence to corroborate or negate these earlier findings and to determine which shunt placement procedure might be superior.
In the present study the overall shunt malfunction rate at 6 weeks postoperatively was significantly higher in patients who underwent mini-laparotomy. By the end of the follow-up period (12 months), however, the difference in overall shunt malfunction between the two surgery groups was no longer significant. Overall shunt malfunction occurred in 18.3% of patients who underwent mini-laparotomy and 15% of patients who underwent laparoscopic shunt placement (p = 0.404). There were no significant differences in the durations of surgery and hospitalization, or in the need for pain management between the two patient groups; however, the authors reported “a trend toward fewer infections and shorter operation times in the laparoscopic cohort.”
What was significant, however, was the difference in distal shunt malfunction. There was no case of distal shunt malfunction (0%) in the laparoscopic shunt placement group, whereas there were five such cases (8%) in the mini-laparotomy group (p = 0.029). Distal shunt malfunction results from malposition of the peritoneal catheter during surgery or later movement of the catheter away from its proper position. Neither occurred in the laparoscopic shunt placement group.
When asked about the take-away message of the study, Dr. Schucht stated “Using laparoscopy for VP shunt placement can decrease the rate of distal shunt failures and is an elegant, feasible alternative to the standard mini-laparotomy approach.”
Story Source:
The above story is based on materials provided by Journal of Neurosurgery Publishing Group. Note: Materials may be edited for content and length.
Journal Reference:
- Philippe Schucht, Vanessa Banz, Markus Trochsler, Samuel Iff, Anna Katharina Krähenbühl, Michael Reinert, Jürgen Beck, Andreas Raabe, Daniel Candinas, Dominique Kuhlen, Luigi Mariani. Laparoscopically assisted ventriculoperitoneal shunt placement: a prospective randomized controlled trial. Journal of Neurosurgery, 2014; 1 DOI: 10.3171/2014.9.JNS132791